A healthcare facility’s cleanliness directly shapes patient trust and regulatory standing. Business owners cannot treat sanitation as a background task delegated without oversight. Every exam room, waiting area, and surgical suite reflects your brand’s discipline and care standards. A dependable medical cleaning service protects patients while supporting compliance with health authorities. The right provider strengthens your reputation, controls liability exposure, and supports long-term operational stability.
Why Medical Cleaning Standards Matter
Medical cleaning standards define how a facility prevents infection and protects patient safety. Healthcare spaces face higher contamination risks than offices or retail stores. Regulatory agencies such as the Centers for Disease Control and Prevention set clear sanitation expectations. Business owners must align cleaning practices with these healthcare-specific standards to maintain credibility and inspection readiness.
Limits of General Commercial Cleaning
General janitorial services focus on visible dirt rather than clinical pathogens. Medical environments require targeted disinfection against bacteria, viruses, and bloodborne contaminants. A medical cleaning service understands dwell time, which means the contact time needed for disinfectants to work. Staff trained in healthcare sanitation clean high-touch surfaces, such as exam tables and light switches, with precision. They also follow structured room-by-room workflows that reduce cross-contamination. Without this expertise, facilities risk inspection failures and reputational harm.
Financial and Legal Risk Exposure
Improper healthcare cleaning increases liability for business owners and practice managers. Health department inspections can result in citations that disrupt operations. Insurance carriers may question claims linked to sanitation lapses. Patient complaints tied to cleanliness often appear in online reviews and referral networks. This public feedback influences prospective patients who research your brand before booking appointments. A qualified provider reduces these risks through documented procedures and measurable quality controls.
Core Traits of a Reliable Provider
A reliable medical cleaning service demonstrates verified training, compliance knowledge, and operational discipline. Professional providers present documentation rather than vague assurances. They align their processes with healthcare regulations and industry best practices. Business owners should evaluate these core traits before discussing pricing or contract length.
Healthcare Training and Certifications
Healthcare-specific training prepares cleaning staff to work in regulated environments. Reputable companies educate teams on infection control and bloodborne pathogen standards. They reference guidance from agencies such as OSHA, which governs workplace safety requirements. Staff members learn proper chemical handling and the use of protective equipment. This training program reduces workplace injuries and contamination risks. Business owners should request written proof of certifications and ongoing education schedules.
Compliance With Health Regulations
Regulatory compliance means following federal, state, and local healthcare sanitation laws. A dependable contractor understands Environmental Protection Agency disinfectant approvals. They also align with CDC cleaning recommendations for clinical spaces. Additionally, they maintain updated safety data sheets for all chemicals used on site. This documentation supports audit readiness during inspections. A cleaning partner who tracks regulatory updates protects your facility from preventable violations.
Insurance and Risk Management
Comprehensive insurance coverage reflects operational maturity and accountability. A credible medical cleaning service carries general liability and workers’ compensation policies. Coverage limits should match healthcare facility requirements, which often exceed standard office thresholds. Business owners must verify certificate status directly with insurers. This verification step prevents coverage gaps during incidents. Strong risk management practices protect your financial stability and professional standing.

Selecting the Right Healthcare Cleaning Partner
Choosing the right healthcare cleaning partner requires disciplined evaluation, not quick comparisons. Medical facilities operate under strict oversight, leaving little room for sanitation errors. A structured selection process helps business owners identify providers with proven healthcare expertise. The following considerations explain what separates a dependable medical cleaning service from a general contractor.
Experience in Healthcare Settings
Experience in healthcare settings reveals how well a contractor handles clinical realities. Medical facilities operate under strict schedules and patient privacy expectations. Cleaning teams must adapt without disrupting clinical workflows. Business owners benefit from partners who understand these operational pressures.
Proven Work With Clinics and Hospitals
Proven healthcare experience shows that a company can perform under regulatory scrutiny. Ask for references from outpatient clinics, dental offices, or surgical centers. Long-term contracts often indicate consistent service quality and client satisfaction. Additionally, review any performance metrics or inspection outcomes tied to previous engagements. This performance history provides tangible evidence of reliability. A contractor familiar with similar facility types adapts more quickly to your environment.
Managing High-Risk Clinical Areas
High-risk areas include operating rooms, isolation rooms, and procedure suites. These spaces require strict cleaning procedures and precise disinfection. A medical cleaning service trains staff to systematically move from low-risk zones to higher-risk areas. They also separate tools for restrooms and clinical rooms to prevent cross-contamination. This structured approach reduces the transmission of infections across departments. Business owners should observe these workflows during on-site evaluations.
Adapting to Specialty Practices
Specialty practices face unique sanitation challenges distinct from those in general clinics. Dental offices manage aerosol-generating procedures that increase airborne risks. Dialysis centers handle blood-exposure incidents that require careful disposal. Ambulatory surgery centers require rapid yet thorough room turnover between cases. A flexible cleaning partner adjusts protocols to each specialty’s requirements. This adaptability supports patient safety while maintaining scheduling efficiency.
Infection Control and Protocols
Infection control protocols outline how a facility reduces pathogen spread through systematic cleaning. Clear procedures replace guesswork with documented accountability. A structured medical cleaning service develops written plans aligned with healthcare guidelines. Business owners should review these plans before finalizing contracts.
Use of Hospital-Grade Disinfectants
Hospital-grade disinfectants target specific pathogens common in medical environments. These products appear on the EPA’s List N for emerging viral pathogens. Staff must follow the correct dilution ratios and dwell times to ensure effectiveness. A reliable provider trains employees to read product labels carefully. This chemical management practice prevents surface damage and ineffective disinfection. Business owners should request product lists and safety documentation for transparency.
Cross-Contamination Prevention Methods
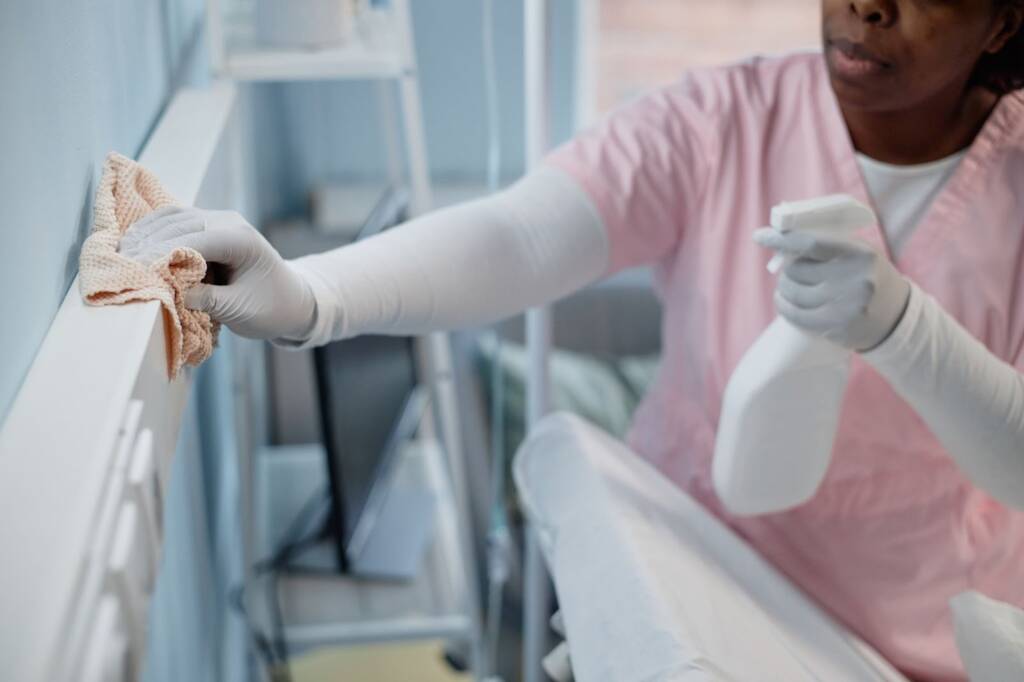
Cross-contamination prevention requires disciplined material handling and sequencing. Professional teams use color-coded microfiber systems for different zones. They replace gloves and sanitize hands between rooms. Additionally, they clean from cleaner surfaces toward more contaminated areas. This directional cleaning method limits pathogen transfer. Clear supervision reinforces these habits across all shifts.
Written Infection Control Plans
Written infection control plans define frequency, methods, and responsible personnel. These documents clarify expectations for daily, weekly, and deep-clean tasks. They also outline emergency procedures for spills or outbreak scenarios. This documentation supports communication between facility managers and cleaning supervisors. Regulatory inspectors often request such records during reviews. A provider who maintains organized plans demonstrates operational discipline.
Staffing and Quality Oversight
Staffing and oversight determine whether protocols translate into consistent performance. A medical cleaning service depends on disciplined hiring and supervision. Screening and training build the foundation for reliable service delivery. Ongoing inspections ensure standards are maintained across shifts and locations.
Employee Screening and Background Checks
Healthcare environments require trustworthy personnel with verified histories. Reputable providers conduct background checks before assigning staff to medical sites. They confirm identity and work authorization status. This screening process reduces security risks for patients and employees—cleaning staff often access facilities after hours, which increases the need for trust. Business owners should request written hiring policies during vendor evaluations.
Ongoing Training and Supervision
Ongoing supervision reinforces correct cleaning practices and safety procedures. Supervisors conduct routine walkthroughs and provide corrective feedback when needed. They update teams on regulatory changes and new disinfectant protocols. This oversight process identifies minor issues before they escalate into inspection concerns. Additionally, structured supervision supports consistent quality across multiple shifts. Reliable providers view supervision as an ongoing responsibility rather than a periodic review.
Inspection and Reporting Systems
Inspection systems create measurable proof of service quality. Many companies use digital checklists to document completed tasks in real time. These reports allow facility managers to objectively verify performance. This reporting structure promotes transparency and shared accountability. Data collected from inspections can reveal patterns requiring operational adjustments. Clear reporting strengthens long-term partnerships between healthcare businesses and cleaning providers.
Data-Driven Cleaning and Performance Metrics
Data-driven cleaning measures sanitation performance using objective, trackable indicators rather than visual impressions. Healthcare business owners benefit from metrics that verify consistency and compliance. A modern medical cleaning service should document tasks, inspection results, and response times in structured systems. Clear performance data supports regulatory readiness while strengthening operational oversight.
Key Performance Indicators in Healthcare Cleaning
Key performance indicators (KPIs) measure how well a cleaning program meets expectations. Common healthcare KPIs include inspection pass rates, task completion accuracy, and response time to urgent requests. Some facilities also track ATP testing results, which measure organic residue on surfaces using light-based detection. This testing method provides numerical evidence of surface cleanliness beyond visual checks. Consistent KPI tracking highlights trends that require correction or retraining. Business owners should review these metrics monthly to maintain accountability.
ATP Testing and Surface Verification
ATP testing offers scientific confirmation of cleaning effectiveness. ATP stands for adenosine triphosphate, a molecule found in organisms such as bacteria and in bodily fluids. Handheld devices swab surfaces and measure light output to estimate contamination levels. Lower readings indicate cleaner surfaces after disinfection. A reliable medical cleaning service uses this tool selectively in high-risk areas, such as exam rooms and procedure areas. This verification method strengthens credibility during inspections and internal audits.
Digital Reporting and Transparency Systems
Digital reporting systems create real-time visibility into cleaning performance. Supervisors log completed tasks through mobile applications or cloud-based dashboards. Facility managers can instantly review timestamped records and inspection notes. This transparency reduces disputes over missed services or incomplete tasks. Additionally, digital records support health authorities’ documentation requests. Structured reporting builds trust between healthcare administrators and cleaning providers.
Using Data to Improve Operational Efficiency
Performance data should guide improvement rather than remain archived. Cleaning companies can analyze recurring deficiencies and adjust training programs accordingly. For example, repeated failures in restroom inspections may signal procedural gaps. Data review meetings between facility managers and contractors strengthen collaboration. This ongoing evaluation process reduces infection risks and operational disruptions. A provider that uses measurable insights demonstrates long-term commitment to healthcare excellence.
Protect Your Health Facility With Expert Cleaning
Expert medical cleaning protects more than surfaces; it protects your reputation and regulatory standing. Healthcare facilities that rely on structured, accountable sanitation programs reduce risk at every level. A qualified medical cleaning service delivers measurable performance, not assumptions about cleanliness. Review your current provider carefully and align your standards with partners who meet the demands of modern healthcare environments.
Stay informed on smarter sanitation strategies and industry updates by reading the latest articles on the Paragon Peak Building Maintenance blog.



